Unprecedented Valuation: Unpaid Family Caregiving Reaches $1.01 Trillion Annually, Prompting Critical 2026 Legislative and Programmatic Relief Efforts

The economic contribution of unpaid family caregivers in the United States has reached a staggering $1.01 trillion annually, according to the newly released AARP Valuing the Invaluable 2026 report. This monumental figure underscores the indispensable role of family members in sustaining the nation’s healthcare infrastructure and supporting millions of older adults and individuals with disabilities. The revelation comes as legislative bodies at both federal and state levels, alongside existing governmental programs, intensify efforts to provide tangible financial relief and recognition to these foundational caregivers. For too long, this labor, often described as a "full-time job for free," has been undervalued, but 2026 marks a pivotal year with new initiatives aiming to funnel real money back into caregivers’ pockets.
The Invisible Workforce: A Trillion-Dollar Foundation
The AARP’s "Valuing the Invaluable" series has for decades shed light on the quiet revolution happening within American households, quantifying the immense care provided by family members. The 2026 report’s finding of $1.01 trillion represents a substantial increase from previous estimates, reflecting both the rising number of individuals requiring care and the growing intensity of the care provided. To put this figure into perspective, it surpasses the combined market value of some of the nation’s largest industries and would rank as one of the world’s largest economies if it were a country. This economic backbone is formed by an estimated 48 million caregivers, many of whom navigate complex medical needs, manage daily living activities, and provide crucial emotional support without formal compensation or adequate systemic support.
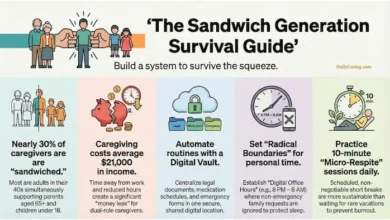
This burgeoning reliance on family caregivers is driven by several demographic and societal factors. The rapidly aging U.S. population, with the cohort of individuals aged 65 and older expanding significantly, inevitably increases the demand for long-term care. Concurrently, rising professional healthcare costs make formal care options—such as nursing homes or in-home professional assistance—prohibitively expensive for many families. This economic pressure often forces families to absorb caregiving responsibilities themselves, leading to a de facto, unpaid extension of the formal healthcare system. Caregivers often provide assistance with activities of daily living (ADLs) like bathing, dressing, and eating, as well as instrumental activities of daily living (IADLs) such as medication management, transportation, and financial oversight. Many also provide complex medical care, once exclusively the domain of trained professionals, including wound care, injections, and operating medical equipment.
A Shifting Landscape: The Evolution of Caregiver Recognition
The journey toward recognizing and compensating family caregivers has been a gradual one, punctuated by advocacy and incremental policy changes. For decades, the societal expectation was that family care was a private matter, an act of familial duty. However, as the demographic realities intensified and the financial strain on caregivers became undeniable, advocacy groups like the AARP and the Alzheimer’s Association began to champion policy changes. Their efforts have aimed to shift public perception and legislative priorities, culminating in the current momentum seen in 2026.

Historically, federal support for family caregivers has been indirect, primarily through tax deductions for medical expenses or dependent care credits that were often insufficient or too narrowly defined. State-level innovations typically preceded federal action, with some states piloting programs to pay family members through Medicaid waivers or offering modest tax breaks. The significant increase in the estimated value of caregiving has served as a powerful call to action, providing concrete data for policymakers to justify more robust legislative responses. This growing body of evidence has been instrumental in framing caregiving not merely as a social issue but as a critical economic component requiring strategic investment.
2026 Initiatives: Pathways to Financial Relief
Against this backdrop of immense value and growing need, 2026 is witnessing a concerted effort to translate recognition into tangible financial support. Several key pathways are emerging or expanding to offer relief:
1. The Federal "Credit for Caring Act" Push:
The bipartisan "Credit for Caring Act" remains a flagship legislative priority in 2026. This proposed federal tax credit aims to provide significant financial assistance, offering a non-refundable federal tax credit of up to $5,000 for working family caregivers. The legislation typically targets caregivers who incur substantial out-of-pocket expenses related to care, such as medical supplies, home modifications, and professional services, and who meet certain income thresholds. Its passage would represent a landmark federal acknowledgement of the financial burden borne by caregivers, offering a standardized national benefit that could alleviate significant strain on millions of households. Advocates, including the Alzheimer’s Impact Movement, emphasize that such a credit would not only ease financial stress but also enable caregivers to remain in the workforce, thereby sustaining their own economic stability while providing essential care.
2. State-Level Success: A Mosaic of Caregiver Tax Credits:
While federal action is debated, numerous states have forged ahead, implementing or proposing their own caregiver tax credits, creating a dynamic patchwork of support across the nation. Oklahoma and Nebraska have emerged as pioneers with active Caregiver Tax Credits, demonstrating a proactive approach to supporting their residents.
- Oklahoma: Its active program offers up to $3,000, notably including medical mileage for all ages, acknowledging a common and often overlooked caregiving expense. House Bill 4118 outlines these provisions, reflecting a comprehensive understanding of caregiving costs.
- Nebraska: Also providing up to $3,000, Nebraska’s credit offers a 50% reimbursement of qualified care expenses, incentivizing the formal tracking of costs.
- North Dakota: With an active credit of up to $4,000, North Dakota specifically targets family members aged 65 and older with lower incomes, directing support to those most vulnerable.
- Georgia: An existing credit offers $750, with legislative discussions focused on expanding its scope and value for 2026, signaling a trend toward increased state investment.
Beyond these active programs, a wave of states has pending legislation for 2026, indicating a growing recognition of the urgency:
- New York: A major proposal (A 09587) envisions a significant credit of up to $6,000, particularly for home modifications and substantial care expenses, reflecting the high cost of living and care in the state.
- Minnesota: Proposed legislation (SF 1114) introduces a "Home Caregiver Credit" of $200 per month, totaling $2,400 annually, providing consistent, ongoing support.
- New Jersey: Senate Bill S1199 proposes a gross income tax credit of up to $2,500 for qualified caregivers, aiming to reduce the tax burden on those providing uncompensated care.
- Massachusetts: House Bill H 3159 seeks to establish a refundable tax credit of $1,500 for uncompensated care, ensuring that even lower-income caregivers can benefit.
- West Virginia: Senate Bill SB 465 focuses its proposed $3,000 credit on medical equipment and respite care, addressing specific high-cost needs.
- South Carolina: Bill 825 proposes a $1,000 credit for intensive care needs per dependent, recognizing the amplified demands of complex care.
- Maryland: A targeted "Caring for Aging Parents" bill aims to provide up to $3,000, signaling a specific focus on elder care within the state.
- Michigan: Newly introduced House Bill HB 5214 indicates an individual income tax credit, with the specific amount yet to be determined, but demonstrating a clear legislative intent.
These diverse state approaches highlight a decentralized but robust movement toward caregiver financial support, often tailored to the specific needs and demographics of each state.

3. Medicaid Self-Directed Services: Getting Paid to Care:
One of the most immediate and impactful avenues for financial relief is through Medicaid Self-Directed Services, often referred to as consumer-directed or participant-directed care. This model empowers individuals who are eligible for Medicaid and require long-term care to manage their own services, including hiring and paying their own caregivers. Crucially, this often allows the care recipient to hire a family member as their personal care assistant.
This mechanism recognizes the existing labor of family caregivers by providing an hourly wage for tasks they are already performing. It shifts the dynamic from unpaid familial duty to a compensated role, providing not only financial remuneration but also a formal acknowledgement of the work’s professional nature. The ability to direct services gives care recipients greater autonomy and choice, while simultaneously providing essential income to family caregivers, often preventing them from having to choose between their loved one’s care and their own financial stability. Each state’s Medicaid program has specific eligibility criteria and administrative processes, but the underlying principle of self-direction offers a powerful model for formalizing and funding family care.
4. 2026 HSA Expansion and Medical Deductions:
The tax landscape for caregivers is also evolving to offer more relief. As of January 1, 2026, new IRS rules have made bronze and catastrophic health plans HSA-compatible. This expansion significantly increases the number of families who can leverage Health Savings Accounts (HSAs) to use pre-tax dollars for qualified medical and caregiving expenses. HSAs offer a triple tax advantage: tax-deductible contributions, tax-free growth, and tax-free withdrawals for qualified medical expenses, making them an invaluable tool for managing healthcare costs.
Furthermore, existing IRS provisions allow caregivers to claim a loved one as a dependent if they provide more than half of that individual’s support and meet other criteria. This can unlock significant tax deductions, particularly for medical expenses that exceed 7.5% of the caregiver’s adjusted gross income. These deductions can cover a wide range of costs, from prescription medications and doctor visits to certain long-term care services, offering a crucial offset to the financial burden. Understanding and strategically utilizing these tax provisions is an essential component of a caregiver’s financial planning.
Empowering Caregivers: A Strategic Action Plan for 2026
For caregivers seeking to transition from providing unpaid labor to receiving deserved financial support, a proactive and organized approach is essential. The new legislation and expanded programs, while a massive win, do not automatically disburse benefits; they require careful documentation and proactive engagement.
1. Build Your Caregiver Paper Trail: Financial relief, particularly through tax credits, hinges on documented expenses. Establishing a dedicated system—be it a physical folder, a digital spreadsheet, or a specialized app—to track all out-of-pocket costs immediately is crucial. This includes receipts for medical supplies, co-pays, home modifications, transportation costs (e.g., mileage logs for medical appointments), respite care, and any other expenses directly related to the care recipient. Detailed records will be indispensable when applying for credits or deductions.
2. Connect with Your Local Area Agency on Aging (AAA): Local Area Agencies on Aging are often underutilized resources. They serve as central hubs for information, referrals, and often manage local grants for respite vouchers, emergency repairs, or other financial assistance programs that may not receive national attention. These agencies can also help navigate state-specific programs and eligibility requirements for Medicaid waivers or other forms of support. A direct inquiry, such as asking, "What respite or financial support programs are available for family caregivers under the Older Americans Act in our county?" can open doors to invaluable local resources.
3. Check for "High-Intensity" Eligibility: Specific caregiving situations often unlock higher tiers of financial relief or specialized programs. For example, caring for an individual with Alzheimer’s disease or other dementias, or someone with severe physical disabilities, may qualify for enhanced benefits due to the increased demands and costs associated with such conditions. Veterans’ caregivers also have specific programs through the Department of Veterans Affairs. Investigating these specialized programs based on the care recipient’s diagnosis or veteran status can lead to substantial additional support.

Broader Impact and Future Implications
The $1.01 trillion valuation is a bittersweet milestone. While it definitively quantifies the monumental contribution of family caregivers, it simultaneously casts a stark light on the profound financial and emotional weight they have carried, often in isolation. This valuation, combined with the emerging legislative and programmatic support in 2026, signals a critical inflection point for American society.
Economic Implications: Recognizing caregiving as a trillion-dollar industry has profound economic implications. It highlights the vast savings to the formal healthcare system and the potential economic fallout if this informal care infrastructure were to falter. Providing financial relief to caregivers can not only improve their personal financial stability but also boost local economies through increased spending power. Furthermore, policies that support caregivers to remain in the workforce, such as tax credits for working caregivers, contribute to broader labor force participation and economic productivity.
Social and Health Implications: The strain of unpaid caregiving often leads to caregiver burnout, mental health challenges, and physical ailments. Financial relief can mitigate some of this stress, potentially improving caregiver well-being and, by extension, the quality of care provided to their loved ones. Addressing the financial burden also begins to tackle the pervasive gender disparities in caregiving, as women disproportionately bear these responsibilities and the associated career and financial sacrifices.
Policy Sustainability and Future Directions: While the 2026 initiatives are a significant step forward, they also raise questions about the long-term sustainability and comprehensiveness of caregiver support. The patchwork of state-level programs, while innovative, creates inequities depending on geographical location. A more robust, integrated federal strategy, potentially building on the "Credit for Caring Act," could provide more consistent and equitable support nationwide. Future policy discussions will likely focus on expanding eligibility, increasing benefit amounts, and exploring innovative models of care that blend formal and informal support more seamlessly. The goal must be to ensure that caregiving is not a path to poverty but a recognized and supported essential service.
The year 2026 stands as a testament to the growing national recognition of family caregivers. Their invaluable work, now quantified at an astounding $1.01 trillion, is finally beginning to receive the tangible financial support it deserves. By strategically engaging with the available and emerging programs—from federal tax credits and state initiatives to Medicaid self-directed services and optimized tax deductions—caregivers can ensure that their essential contributions are not only appreciated but also appropriately compensated. This is more than just "helping out"; it is performing essential work, and it is time for that work to be financially acknowledged and supported.