Employer-Sponsored Health Insurance 101
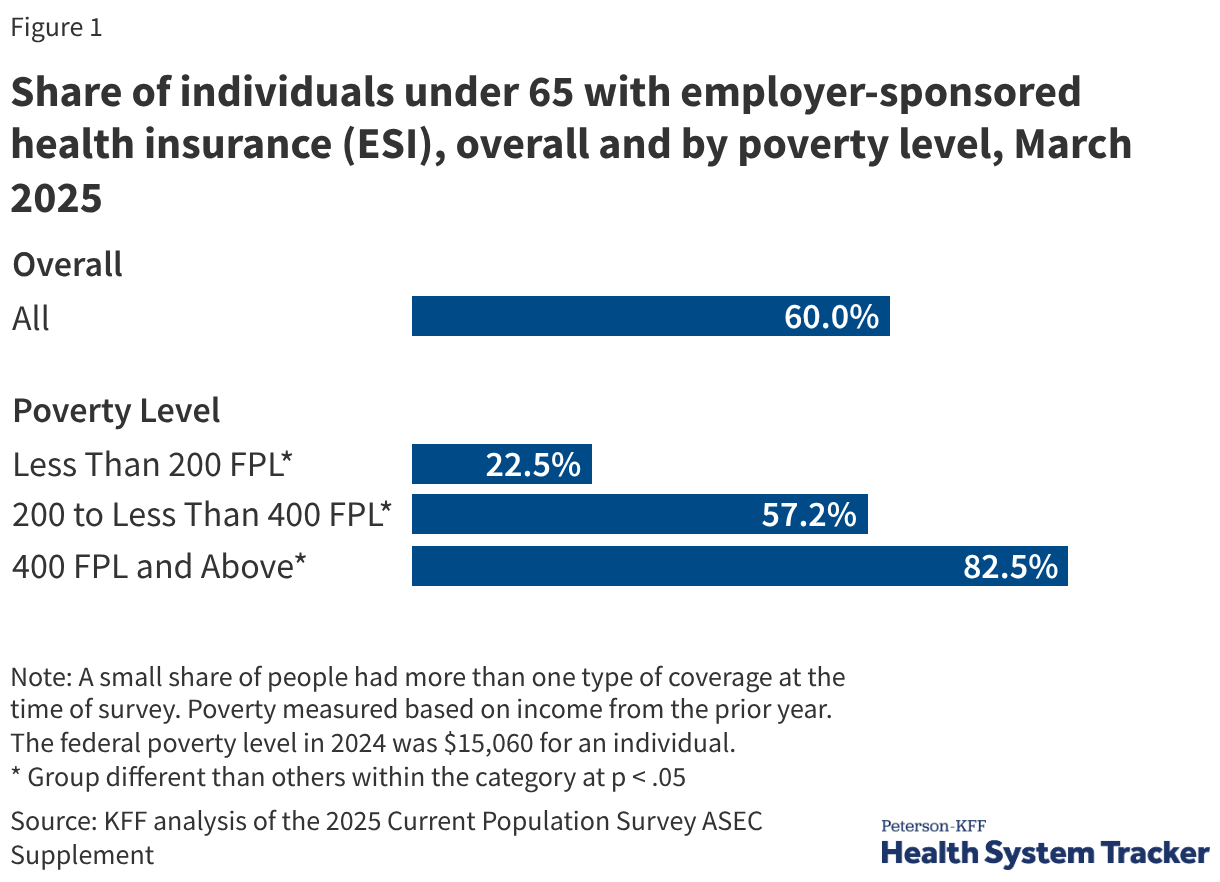
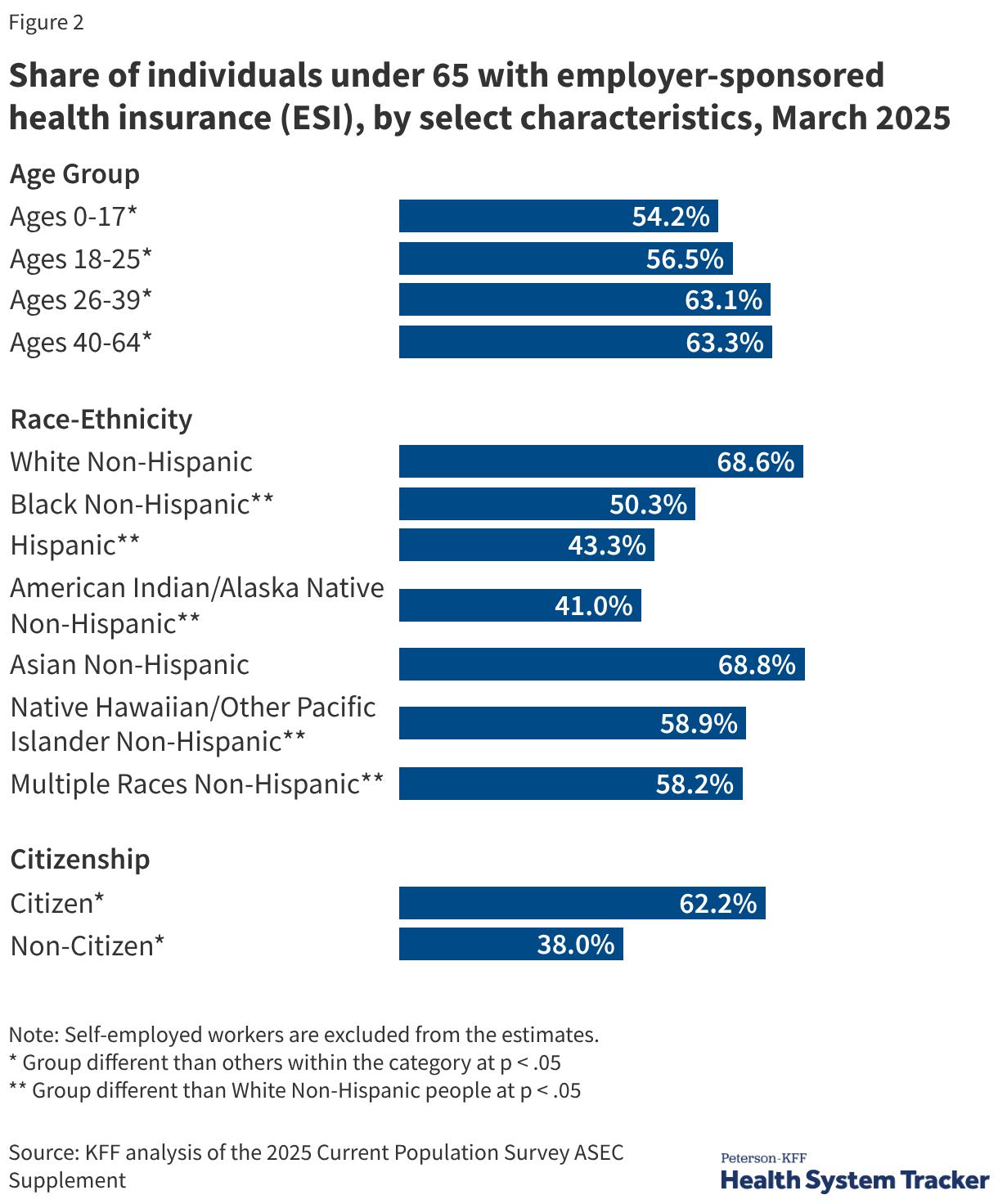
Employer-sponsored health insurance (ESI) remains the foundational pillar of the United States healthcare system, serving as the primary source of coverage for the vast majority of Americans under the age of 65. As of March 2025, approximately 165.6 million people—representing 60% of the non-elderly population—rely on health plans provided through their place of employment. Unlike many other developed nations that utilize centralized or single-payer systems, the U.S. model is built upon a voluntary, private framework that incentivizes employers to provide coverage through significant tax advantages and administrative efficiencies. However, while ESI offers a streamlined path to care for millions, the system is characterized by deep disparities in access and affordability, particularly for low-wage earners and those employed by small businesses.

The Structural Framework of Employer-Sponsored Coverage
In the U.S. market, private health insurance is generally acquired through two avenues: the individual market (often via the Affordable Care Act’s Healthcare.gov) or group health insurance provided by an employer, union, or trade association. Within the ESI framework, the term "insurance" can be technically nuanced. Employers typically fund these benefits in one of two ways. Under an "insured plan," the employer purchases a policy from a state-licensed insurer like Aetna or UnitedHealthcare. Conversely, many large organizations opt for "self-funded plans," where the employer pays for healthcare claims directly from its own assets, often protected by "stop-loss" insurance to mitigate the risk of catastrophic claims.
These plans are governed by the Employee Retirement Income Security Act (ERISA) of 1974. ERISA establishes a federal structure for disclosure and fair dealing, ensuring that private employers meet specific obligations to their enrollees. Notably, ERISA does not apply to public sector plans or church-sponsored programs, creating a bifurcated regulatory landscape. Furthermore, the market is divided into "small group" (typically fewer than 50 or 100 employees) and "large group" segments, with small group plans generally facing more stringent state-level benefit requirements.

A Chronology of Employer-Sponsored Insurance in America
The dominance of ESI in the United States is not the result of a single legislative act but rather an evolution of wartime policy and subsequent tax law.
- 1942: The War Labor Board Decision. During World War II, the federal government froze wages to prevent inflation. To remain competitive in a tight labor market, employers began offering fringe benefits, including health insurance, which were not subject to the wage freeze.
- 1954: Internal Revenue Code Enactment. Congress formally codified the tax-exempt status of employer-paid health insurance premiums. This solidified the workplace as the primary hub for medical coverage.
- 1974: Passage of ERISA. Federal oversight was established to protect employee benefits, though it also allowed large employers to bypass varied state insurance mandates through self-funding.
- 2010: The Affordable Care Act (ACA). The ACA introduced the "employer mandate," requiring firms with 50 or more full-time equivalent (FTE) employees to offer affordable, high-value coverage or face financial penalties.
- 2023: The "Family Glitch" Fix. New federal rules addressed a long-standing loophole that prevented dependents from accessing Marketplace subsidies if a worker’s self-only coverage was deemed "affordable," even if family coverage was not.
- 2025: Current Market State. ESI reaches a record cost threshold, with average family premiums nearing $27,000 annually.
The Economic Engine: Tax Preferences and Risk Management
The persistence of ESI is driven by two powerful economic factors: administrative efficiency and massive federal tax subsidies. From a risk management perspective, the workplace is an ideal environment for insurers. Because people generally choose jobs based on their profession rather than their health status, employer groups provide a "normal" mix of healthy and less-healthy individuals. This reduces "adverse selection," where only those with high medical needs seek coverage, which would otherwise drive premiums to unsustainable levels.
Furthermore, the tax treatment of ESI represents one of the largest "tax expenditures" in the federal budget. Unlike cash wages, employer contributions toward health premiums are not subject to federal income or payroll taxes (Social Security and Medicare). In 2022 alone, this exclusion cost the federal government an estimated $312 billion in foregone revenue. For an employee in the 22% tax bracket, a dollar of health benefits is worth significantly more than a dollar of wages, which would be reduced by nearly 40% after income and payroll taxes are deducted. While critics argue this encourages the "over-consumption" of healthcare, the subsidy remains a politically sacrosanct component of the American social contract.
Analyzing 2025 Market Data: Premiums and Deductibles
The cost of maintaining this system continues to climb, placing a strain on both corporate balance sheets and household budgets. In 2025, the average total premium for a single worker reached $9,325, while family coverage for a household of four hit $26,993. On average, employers cover 84% of the premium for single coverage and 74% for family coverage.
However, the "sticker price" of the premium is only one part of the financial burden. To keep premiums manageable, many employers have shifted costs to workers through higher deductibles.
- Deductible Growth: In 2025, 88% of covered workers face a general annual deductible. The average deductible for single coverage stands at $1,886, but this figure spikes to $2,631 at smaller firms.
- The $2,000 Threshold: Approximately 34% of all covered workers now have a deductible of at least $2,000, up from 26% five years ago.
- Out-of-Pocket Maximums: While the ACA caps total spending, 21% of workers still face an out-of-pocket limit exceeding $6,000 for single coverage, a figure that can be devastating for low-wage households.
The Diversity of Plan Types and Network Strategies
Modern ESI is no longer a one-size-fits-all model. Workers typically choose between several distinct plan architectures:
- Preferred Provider Organizations (PPOs): The most common plan type, offering broad networks and the ability to see specialists without a referral.
- Health Maintenance Organizations (HMOs): More restrictive plans that generally do not cover out-of-network care and require "gatekeeping" by a primary care physician. HMO enrollment has declined from 30% in the late 1990s to roughly 12% today.
- High-Deductible Health Plans with Savings Options (HDHP-SOs): These plans pair a high deductible with a tax-advantaged Health Savings Account (HSA). Nearly 30% of workers are now enrolled in these plans, which are designed to make enrollees more "price-conscious" consumers of care.
To control costs, employers are increasingly utilizing "narrow networks" or "tiered networks." In these models, insurers select providers based on quality and cost efficiency. Enrollees pay less when they visit "Tier 1" or "Centers of Excellence" providers. While these strategies can lower premiums, they often face pushback from employees who value broad choice and established doctor-patient relationships.
Access Disparities and the "Family Glitch"
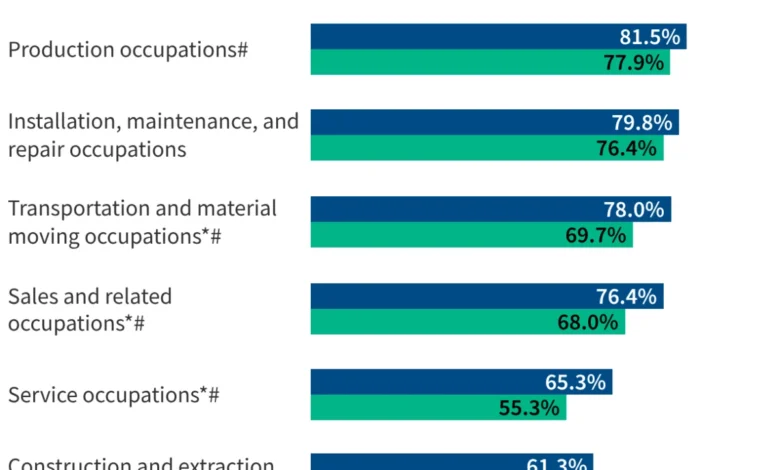
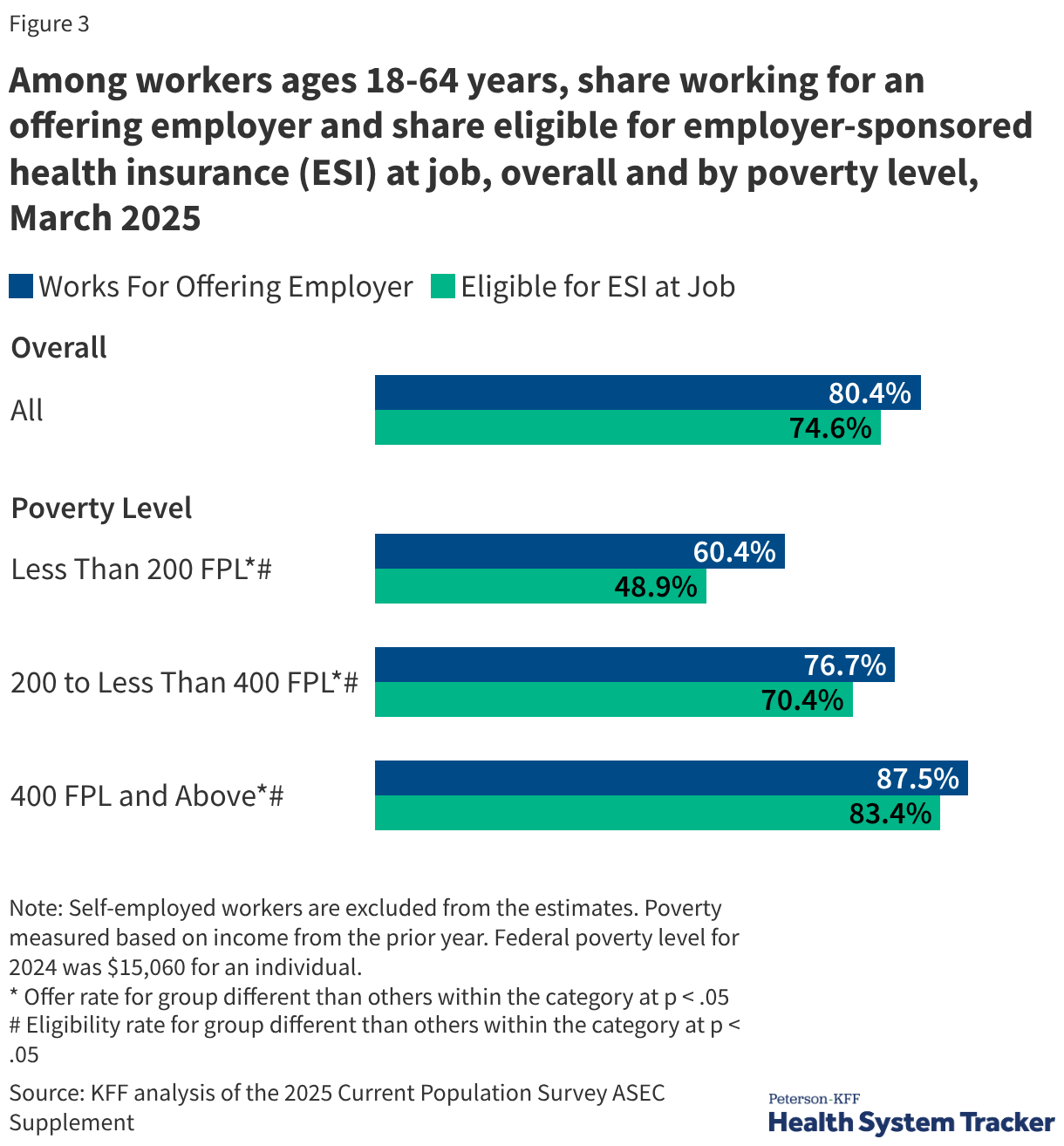
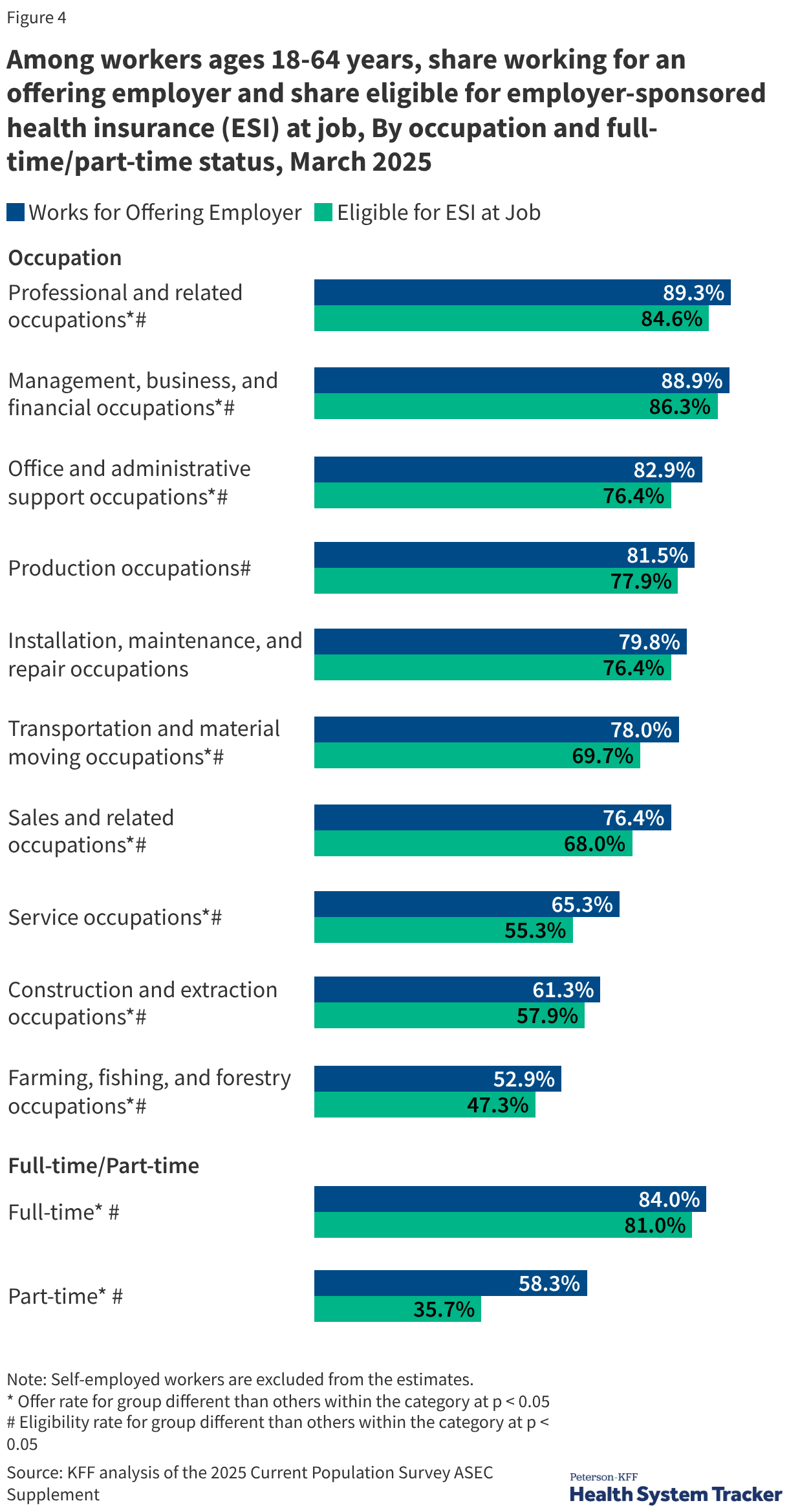
Despite the ubiquity of ESI, access is highly correlated with income and firm size. Among workers earning at least 400% of the Federal Poverty Level (FPL), 87.5% work for an employer that offers coverage. For those earning less than 200% of the FPL, that number drops to 60.4%. Furthermore, eligibility remains a hurdle; part-time and seasonal workers are frequently excluded from benefits even when their employer offers them to full-time staff.
The "family glitch" fix of 2023 was a landmark regulatory change intended to improve access for low-income families. Previously, if an employer offered "affordable" coverage for the individual worker, the entire family was barred from receiving subsidies on the ACA Marketplace, even if the cost to add the family to the employer plan was 20% or 30% of their income. Current rules now evaluate the affordability of family coverage separately, allowing millions of dependents to seek more affordable options through government-subsidized exchanges.
Official Responses and Future Outlook
Industry groups and policymakers are currently grappling with the friction points of the ESI system. A significant area of concern is the complexity of "prior authorization," a utilization management tool where insurers must approve services before they are performed. In early 2025, major insurers issued a voluntary pledge to expedite these processes following widespread complaints from patients and providers regarding care delays.
From a policy perspective, the introduction of new price transparency rules is expected to reshape how employers negotiate with hospitals. By forcing the disclosure of negotiated rates, the federal government aims to empower employers to identify high-cost providers and steer enrollees toward higher-value care.
As the U.S. looks toward the latter half of the decade, the sustainability of ESI faces several critical questions:
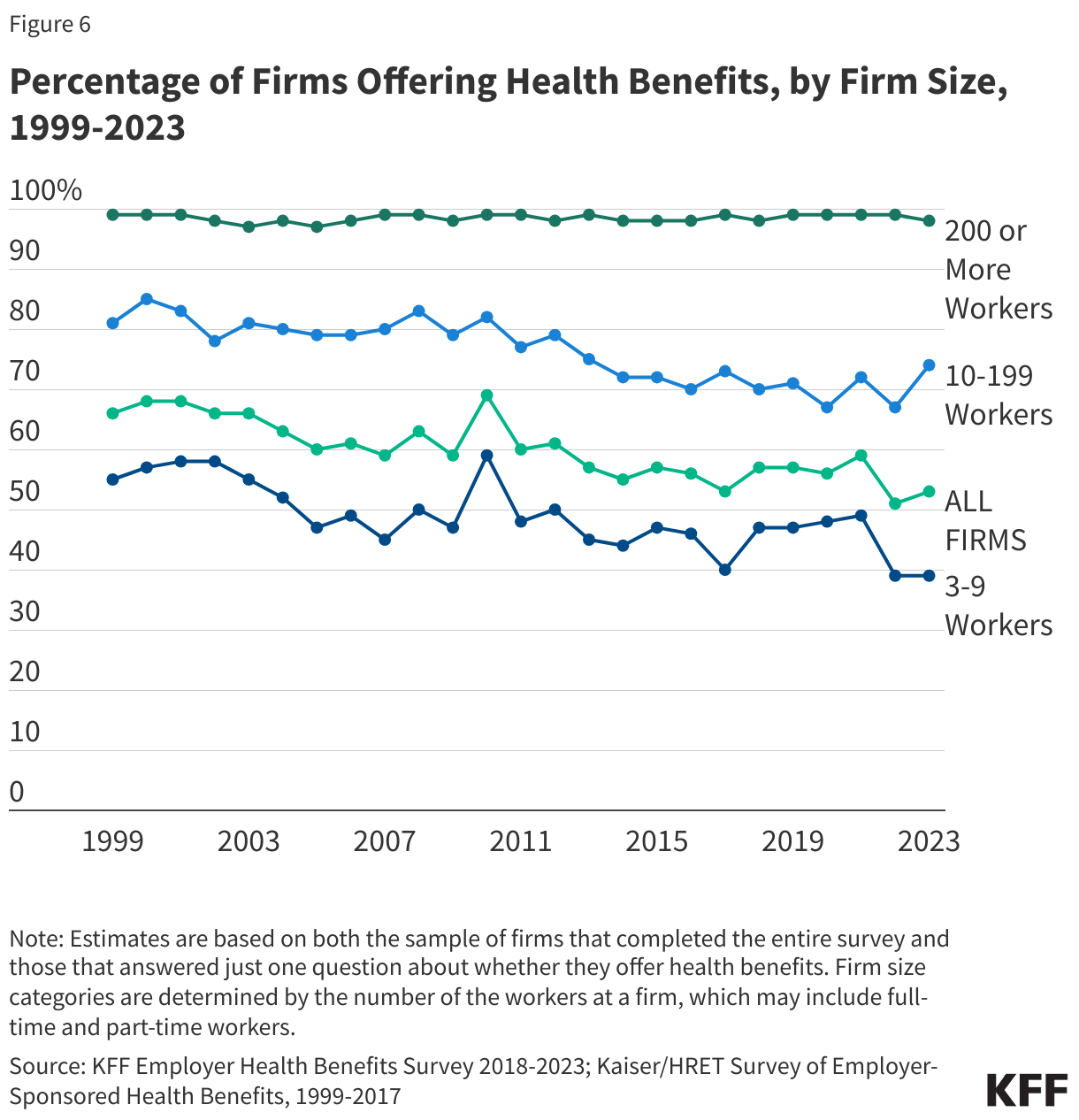
- The Low-Wage Gap: With only 50% of low-income workers currently eligible for ESI, can the system truly claim to be the primary safety net for the working class?
- Mental Health Parity: While 92% of firms believe they offer timely access to primary care, only 70% say the same for mental health. Closing this gap remains a top priority for regulators and labor advocates.
- Cost Shifting Limits: There is growing concern that deductibles have reached a "breaking point" where enrollees skip necessary care to avoid out-of-pocket expenses, potentially leading to higher long-term costs.
Ultimately, employer-sponsored health insurance remains a uniquely American compromise—a blend of private-sector competition and massive public-sector subsidy. While it provides stability for over 165 million people, its future depends on the ability of employers and insurers to rein in costs without sacrificing the financial security of the American worker.